 UK Nurse: My Experience Of Working Through The 2014 Ebola Crisis
UK Nurse: My Experience Of Working Through The 2014 Ebola Crisis23 Jun 2021 ● Katy Pitt-Allen, Adult Nurse
UK Nurse: My Experience Of Working Through The 2014 Ebola Crisis
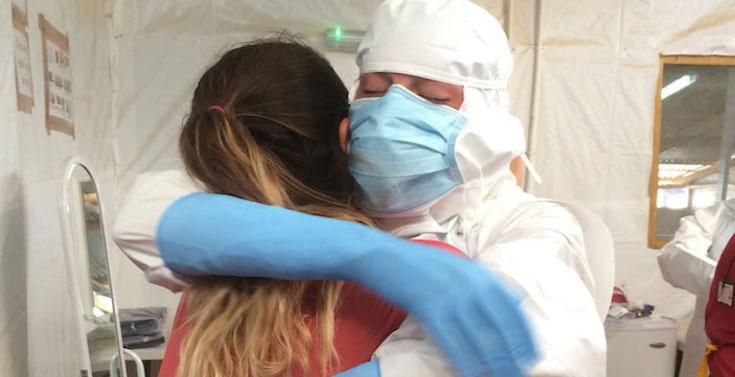 "Even reflecting back on this now, 6 years on, the trauma of what we all experienced and the desperation these people felt, is raw."
"Even reflecting back on this now, 6 years on, the trauma of what we all experienced and the desperation these people felt, is raw."Katy discusses her time working in West Africa during the 2014 Ebola epidemic, offering insights into the psychological toll of a viral outbreak, and the parallels with the current global pandemic.
Topics covered in thsi article
Introduction
It was late 2014 and I had just come back from a busy shift at the hospital, having braved the cold December rain.
I was tucked up in the front room of our little house in Bristol reeling from the predictable ‘Winter pressures’ we were facing on the ward.
My husband suggested we watch a BBC 2 documentary about the Ebola outbreak in West Africa.
Little did I know, the next 40 minutes would drastically alter my course for the next year.
My passion for equality in healthcare is what has driven me, and I remember the sadness and shock that I felt watching the footage of the people of West Africa, arriving desperate and terrified at various field hospitals set up across Sierra Leone, Guinea and Liberia.
I remember the fierce need I felt to be able to do something, I just didn't know how.
So, it felt like fate when that week an email arrived in my work inbox appealing for NHS volunteers to deploy as part of an Ebola response program.
The Application Process
I hit the reply button immediately, sending over my CV and a brief cover letter.
If I'm honest, I didn't really expect a response at all, let alone immediately.
So I was quite shocked when I was scheduled for a phone interview the following week.
I had no idea what to expect or indeed what was expected of me so it was very nerve wracking.
The phone interview was 1 hour and consisted of lots of clinical scenario questions.
I felt like my experience in a busy ward, triaging emergency patients contributed to my ability to be able to think on my feet.
The next day I was informed that I would be on an upcoming deployment, headed straight for Freetown, Sierra Leone.
I felt exhilarated and terrified.

After keeping my application process relatively secret up until that point, it was In November 2014 that I broke the news to my family that I had been accepted to join NHS Nurses and Doctors from all over the country to respond to the Ebola pandemic... and there was a possibility of me being in Sierra Leone for Christmas.
In December I went to the London school of tropical medicine to attend an information session and was then informed of my deployment date 03/01/2014.
However, there were still many obstacles to overcome.
As 1 of 3 Senior Staff Nurses on a busy ward, to say I had to negotiate my release was an understatement.
After what felt like a long and disappointing negotiation with senior members of the hospital it was ultimately decided that during a particularly challenging winter, I was of more value on the ward and they were unable to release me until February, at least.
I was incredibly disappointed, but little did I know that Ebola would still be tearing through West Africa until early Spring and my call up would come.
After a full medical, what felt like a million vaccinations, psychiatric assessments and a mountain of emails, I received my deployment date, February 6th 2015 - my fiancé’s 30th birthday.
Pre-Deployment Training
I packed my bags and said goodbye to friends (whilst leaving little gifts for my husband to find on his birthday).
I felt the most overwhelming sense of pride, but I was also hyper aware that I really was stepping into the unknown, and I could only hope that my so far short career in an inner city hospital had prepared me somewhat.
There were approximately 22 of us selected to deploy to West Africa on February the 6th and we all had to attend a week of intense pre-deployment training prior to departure.
We met at a Premier Inn which would be our home for the next 7 days.
I said goodbye to my husband to be and walked into the hotel foyer where I was greeted by the people that I would be working alongside at some of the most challenging points of our medical careers.

Anaesthetists, Nurses, Paediatricians, Dr’s and Pharmacists, we were all there for the same reason, packed and ready for the complete unknown.
Our pre departure course was intense, 10 hour days of PPE training and assessment, cultural awareness, how to recognise Ebola, how to treat and manage, how to work in a field hospital...
The amount of information was completely overwhelming.
We were also all trying to form professional bonds with a team of people that our safety would depend on.
It was totally surreal.
PPE
During the training course Donning and Doffing (putting on and taking off) the PPE was assessed at every point, your reaction to it - the ability to put it on, work in it, not panic.
You see the PPE comprised of 8 steps minimum and that doesn't include washing your hands thoroughly according to the 7 steps process.
So as you can imagine there was a lot to remember - a slip up at any point could mean that you have exposed yourself to the Ebola virus.

In 2015 there was no cure for Ebola, there was relatively little treatment - all you were able to offer was supportive care and hope that the body did not go into multi organ failure.
There was a high fatality rate - It infected and killed indiscriminately.
It goes without saying that your PPE, the only thing between you and Ebola, was vital and during the donning and doffing drills there was usually a heavy silence.
The PPE practice was akin to an army drill, over and over and over again until the assessors were confident that you were able to do it in adverse conditions.
Departure
On the morning of the 6th Feb we all headed to Heathrow.
We had been split into 2 groups and once we reached Sierra Leone we would be headed to the opposite sides of the country.
I would be working in a team of 11 going to an army field hospital called Kerry Town - with ‘Save the Children’.
After a long flight, we arrived into Freetown, it was the middle of the night and I will remember that journey for the rest of my life.
It felt as if we had touched down in a war zone.
After driving from the airport we were transported by boat to a hotel where we were processed before being bused to our field hospital locations.
We had a week of overlap with the previous volunteers, they were able to show us the ropes and make sure that we felt confident in taking over from them.
When we arrived there was actually a dip in numbers, we wrongly presumed that we would be in for a quiet 6 weeks.
Again, the PPE training was paramount and infinitely harder as temperatures climbed to 40+ degrees.
What Is Ebola?
Ebola is a haemorrhagic fever.
It is transmitted from human to human through bodily fluids.
This includes the bodily fluids of someone who has died from Ebola.
Ebola has more than a 50% fatality rate and survival depends on early supportive treatment.
The symptoms of Ebola include minor flu like symptoms, which will then progress into vomiting, diarrhoea, internal and external bleeding.
In West Africa, it was because of this that nurses and Dr’s died.
In countries with poor sanitary symptoms, close communities and funeral practices that include washing the bodies, controlling the spread of Ebola was incredibly challenging.
Kerry Town Treatment Centre
Kerry Town Treatment Centre was a large 80 bed field hospital.
Purpose built by the army to treat patients with Ebola.
It was just outside of the capital Freetown.
It was here that we would spend our days, Kerry town was split into Red and Green areas.
Most was green - where you were able to walk around freely.
But the wards - were Red.
In the Green zones you were able to walk around in scrubs and wellies.
It was run much like a normal A&E, we would have a handover at the start of each shift where we would discuss PCR (diagnostic test) results and differential diagnoses - we would assign work according to skill sets and start our day.
There were many challenges, one being that you were only able to be in full PPE for a maximum of 2 hours, and once in there you could only move in one direction so as to avoid any cross contamination.
The work was exhausting.
It was 40 degrees, there was no air flow and you were moving around in 4 layers of plastic.
You could barely breathe after 30 minutes as the sweat would start dripping into your mask.
The goggles would dig into the side of your head, causing an almost instant headache.
You moved slowly and deliberately.
By the time you left the Red zone, you had lost anywhere between 1-3 litres of water.
Hyponatremia was a regular occurrence and we all lived on fizzy drinks and isotonic fluids.
There were a lot of rules - one being that It was forbidden to enter the red zone without a ‘buddy'.
This was to ensure your safety at all times as It was not unheard of to tear your PPE on a bed, needle stick injuries and near faints happened.
Trying to cannulate with goggles and 4 pairs of gloves on was difficult to say the least.

When we opened the door to the red zone the first thing was to take in your surroundings.
There were children, babies, and adults everywhere, on beds, on the floor, in doorways.
You were acutely aware that you had limited time, so you had to choose the high priority patients.
Change bed sheets, put up fluids, give pain relief, call the sanitation team to remove the patients that had died.
Even reflecting back on this now, 6 years on, the trauma of what we all experienced and the desperation these people felt, is raw.
Once you made your way out of the red zone it was time to Decontaminate.
This involved being sprayed with chlorine, whilst you slowly and methodically removed all your PPE.
This process would take at least 20 minutes and was the point where you were putting yourself at highest risk.
Your PPE was covered in Ebola virus, and you had to remove it without getting any on you.
It was the most stressful part of it all.
We did this day in, day out for 6 weeks.
We were also so lucky to be able to work with the local Drs and Nurses, they had been there since the beginning - many of them had lost colleagues, friends and families.
Yet they would come to the treatment centre and put themselves at risk every day, until the Ebola epidemic subsided.
Happy Times
There were happy times, where patients recovered, the Nurses and Drs would sing, and clap and we would celebrate the miracle of them walking out of a treatment centre.
These were the times that carried us through, to the next.

Despite these small celebrations the fear surrounding Ebola in these countries did not help, people would delay coming to the hospitals, they were scared.
They had heard terrifying stories of friends and families arriving at the treatment centre never to leave.
Sadly, this was true.
Families, husbands, wives and even children would be separated according to whether or not they were positive or not.
Home
After our 6 weeks in Kerry Town it was time to leave.
We left with heavy hearts but also were keen to get out of there and get back to real life.
It was at this time that we became aware of the amount of monitoring we would be put under.
All of us, were to quarantine for 3 weeks (the incubation time for Ebola) it was during this time that we would receive twice daily phone calls of Public Health England.
We would have to take our temperatures every morning and every evening.
We were discouraged from sharing living spaces if possible and were subject to psychiatric evaluation.
They wanted to know if there was anything we wanted to talk about, where do you start.
What Happened Next
Despite a few scares none of us contracted Ebola and we soon went back to our day jobs, the experience became absorbed into our psyches and we continue to move forward.
I continued to plan my wedding and got married in 2015 of that year.
6 years on and I remember the people of Sierra Leone and my team every day, but it has only been under the harsh light of the current coronavirus pandemic that I have been forced to reflect on my experience, and what it means going forward.

When a health care emergency happens, it takes a strong resilient healthcare system to withstand it, to deliver and provide.
More than I ever did, I believe in national health and equal healthcare for all.
It is an absolute privilege to be able to be part of it and I hope that this time of uncertainty will inspire the most valiant of nurses to step forward and say yes.


